Anemia and stunting are two pressing global health issues that disproportionately affect women, particularly in low- and middle-income countries. Both conditions have profound consequences for maternal health, child development, and overall well-being. Understanding the intricate link between anemia and stunting is crucial for implementing effective interventions and improving women's health outcomes worldwide.
Anemia and Its Impact on Women's Health
Anemia, characterized by a deficiency of red blood cells or hemoglobin in the blood, is one of the most prevalent nutritional deficiencies globally. Women of reproductive age are particularly vulnerable to anemia due to factors such as menstrual blood loss, pregnancy, and inadequate dietary intake of iron and other essential nutrients.
The consequences of anemia in women extend beyond fatigue and weakness. It can lead to adverse outcomes during pregnancy, such as preterm birth, low birth weight, and maternal mortality. Anemic women are also more susceptible to infections, decreased cognitive function, and reduced work productivity, exacerbating the cycle of poverty and inequality.
Stunting and Its Implications for Women
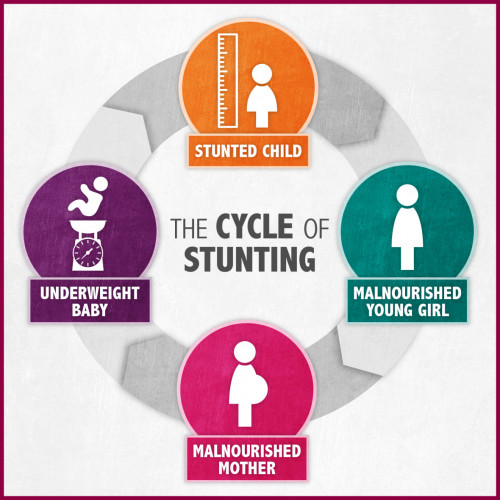
Stunting, a form of chronic malnutrition characterized by impaired growth and development in children, is closely linked to maternal health and nutrition. Women who experienced stunted growth during childhood are more likely to give birth to low-birth-weight babies, perpetuating the intergenerational cycle of malnutrition.
Poor maternal nutrition, inadequate prenatal care, and limited access to nutritious food contribute to the high prevalence of stunting among children born to undernourished mothers. Stunted growth in early childhood not only affects physical development but also has long-term consequences for cognitive development, educational attainment, and economic productivity in adulthood.
The Interconnection Between Anemia and Stunting
The relationship between anemia and stunting is bidirectional and multifaceted. Anemic women are more likely to give birth to stunted children due to the adverse effects of maternal anemia on fetal growth and development. Conversely, stunted children are at higher risk of developing anemia later in life, perpetuating the cycle of malnutrition across generations.
Iron deficiency, a leading cause of anemia, is also implicated in stunting and impaired cognitive development in children. Iron is essential for proper growth, brain development, and immune function, highlighting the critical role of maternal nutrition in preventing both anemia and stunting.
Addressing Anemia and Stunting Through Women's Empowerment
Empowering women is key to breaking the cycle of anemia and stunting and improving overall maternal and child health outcomes. Access to education, reproductive healthcare, nutritious food, and economic opportunities can enhance women's nutritional status and enable them to make informed decisions about their health and well-being.
Integrating nutrition-sensitive interventions into existing maternal and child health programs is essential for addressing the complex interplay between anemia and stunting. Promoting exclusive breastfeeding, micronutrient supplementation, diversified diets, and iron fortification of staple foods can help prevent and alleviate both conditions, benefiting women and their children alike.
Regular hemoglobin screening is crucial in monitoring the effectiveness of treatment interventions for anemia. By tracking hemoglobin levels over time, healthcare providers can assess the response to therapy and make necessary adjustments. This helps ensure that treatment effectively addresses the underlying causes of anemia and promotes the production of healthy red blood cells. Treatment adjustments can be made quickly to optimize outcomes and improve overall well-being.
Conclusion
The link between anemia and stunting underscores the urgent need for holistic approaches to women's health and nutrition. By addressing the underlying determinants of malnutrition and empowering women to take charge of their health, we can break the intergenerational cycle of poverty and improve the lives of millions of women and children worldwide.